Since February is the month of love, I’m here to profess undying love for my professional soulmate – the heart. I can’t help it, I love everything about the heart: the structure, how it works as both its own organ and to keep other organs alive, and the complexity of deciphering procedure reports and assigning codes. It’s no secret to my coworkers that I would rather code my way through a huge stack of cardiac charts than code a few cases of other medical specialties that have failed to capture my heart. And like some lovesick puppy who happens across someone who has sworn off love forever, my heart breaks a little bit when I hear someone say, “I hate coding hearts.” I want to make it my life’s mission to get everyone to feel that same appreciation for this vital organ.
For me, love of the heart comes with understanding its structure and function. I first felt that twinge of amazement in anatomy lab while dissecting a sheep’s heart as I slid glass rods through the valves to see where they would come out. I want you to feel that same amazement. So, let’s get started by taking a closer look at the general anatomy of the heart – without the formaldehyde.
The heart is a hollow organ that is responsible for pumping blood to the lungs, where oxygen is absorbed and carbon dioxide is expelled, and then routing that oxygenated blood to the rest of the body. The first step in coding any cardiac procedure is understanding the structure of the heart and how it works. This is particularly important when coding cardiac catheterization and coronary angiography procedures in ICD-10-PCS.
There are two sides to the heart – right and left – and each side has one atrium and one ventricle. These cardiac chambers pump blood throughout the body. Blood enters the heart through the right atrium and then travels to the right ventricle. It then leaves the heart in a closed circuit to travel to the lungs, where carbon dioxide is exchanged for oxygen. Blood is returned to the heart in the left atrium and then flows through the left ventricle before leaving the heart and pumping blood to the rest of the body.
Cardiac catheterization involves placing a catheter inside the heart and taking blood samples or blood pressures (hemodynamics). The intent of the procedure is to measure blood pressures and take samples (root operation Measurement). Heart catheterization can be done on the right or left side – or both. The side of the heart depends on the reason for the procedure.

The approach for right heart catheterization is through a vein: veins lead to the inferior and superior venae cavae, which empty into the right atrium. The right side of the heart leads to the pulmonary arteries, which deliver oxygen poor blood to the lungs. Indications for right heart catheterization include congestive heart failure, pulmonary hypertension, kidney disease, shock, tricuspid or pulmonary valve disease, and congenital heart conditions.
The approach for left heart catheterization is usually an artery, although it can be accessed from a vein with a transseptal puncture from the right side of the heart (via a venous approach). Arteries lead to the aorta, which leads to the left ventricle. Indications for left heart catheterization include coronary artery disease, aortic or mitral valve disease, cardiac tumors, ventricular septal defects, ventricular dysfunction, and congenital heart disease.
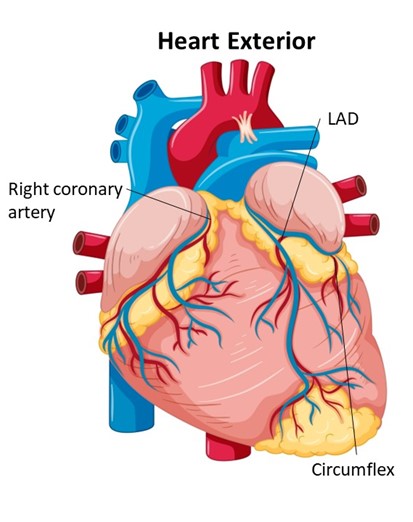
The Outside of the Heart
While the heart chambers make up the inside of the heart, the coronary arteries are located within the muscular heart wall. As blood leaves the heart chambers, the first body part to receive a fresh supply of oxygenated blood is the heart itself. It receives this oxygenated blood from the coronary arteries. The right and left coronary arteries branch off the aorta and wrap around the heart. The left main coronary artery is a short vessel that almost immediately branches into the left anterior descending (LAD) and circumflex arteries. The LAD is a major vessel that oxygenates the left ventricle, the largest heart chamber that is responsible for pushing blood out to the rest of the body.
Blockages in the coronary arteries can cause ischemia (inadequate blood supply) and/or infarction (local tissue death). Obstruction within the LAD can be catastrophic, causing myocardial infarction (heart attack) that has been termed “the widow maker.”
Imaging of Heart Chambers, Coronary Arteries, and Great Vessels
Heart and coronary imaging are often performed in a cardiac cath lab by injecting contrast material into the structure to be viewed. As the contrast mixes with blood, fluoroscopy gives the physician a motion picture-style radiograph (root operation Fluoroscopy). Various structures can be imaged and may be performed with or independent of heart catheterization.
Left ventriculography is the injection of contrast material into the left ventricle. It allows the physician to assess cardiac output and left ventricular wall mobility. Other cardiac chambers may also be injected for imaging but left ventriculography is by far the most common.
The intent of coronary angiography is to inject contrast material into the coronary arteries to identify areas of obstruction. Coronary angiography is often performed in conjunction with cardiac catheterization, but it can be performed independently without the catheter ever crossing the aortic valve to reach the left ventricle. It can identify flow limiting lesions within the coronary arteries and is often the basis for performing percutaneous coronary interventions (PCI), such as angioplasty and stenting.
Want to Learn More?
I could go on (yes, there’s more!), but this blog clearly doesn’t express my passion for the heart as well as I do IRL, so please join me for my webinar, “Considering Cardiac Caths,” where I delve deeper into heart anatomy and cardiac cath-based procedures, including everything discussed above, how your heart is like a house, percutaneous interventions, and more!

Kristi Pollard, RHIT, CCS, CPC, CIRCC, AHIMA-Approved ICD-10-CM/PCS Trainer
Director of Coding Quality & Education<br />
Kristi is the Director of Coding Quality & Education with more than 25 years of industry experience; she is responsible for the development of web-based, instructor-led, and webinar training materials; conducting training in ICD-10-CM/PCS and CPT; and performing DRG and APC audits. Kristi has an extensive background in coding education and consulting and is a national speaker and published writer on topics related to ICD-10 and CPT coding and code-based reimbursement. She has designed and developed training programs for inpatient and outpatient hospital-based coding, with a focus on vascular interventional radiology, interventional cardiology, orthopedics, and obstetrics.


0 Comments